An improved and new Advazorb hydrophilic foam dressing
Written by: Professor Linda Rafter Honorary Professor in Nursing Mary Seacole Research Centre De Montfort University Leicester, Wound Care Solutions Tissue Viability Nurse Consultant
Introduction
This poster reports the progress of three patients employing the Advazorb foam dressing and the results. The Advazorb foam dressing is a soft conforming hydrophilic foam designed to absorb fluid, while retaining it inside the dressing to promote wound healing.
Method
Three patients were recruited from the inpatient and outpatient clinic in the general hospital. Ages ranged between 17 – 90 years. Ward staff nominated patients, who I asked to volunteer in a trial for Advazorb foam dressing. I requested a contact number if they were going home so I could follow the patient up 14 days later. If they were still an inpatient, I visited the ward to perform the follow up information. Opinions of 10 nursing staff were collected on how they felt the Advazorb foam dressings performed. Each patient had at least 14 days treatment to enable an evaluation of the patient’s comfort and whether healing had been successful.
Case Study 1
Mr C, a 63 year old male, had a right knee replacement on 27th May 2011. He was referred to the author after a washout in theatre on 1st June 2011, due to infection and an increased pain. He is known to have rheumatoid arthritis. On assessment the lateral end of the knee, wound was 3cms deep and bleeding clips were still in situ. His serum albumin was 22, Hb 8.2, white cell count 7.6, Waterlow score 7, BMI 27 and Must 0. He had a period of treatment with topical negative pressure dressings from 17th June 2011 to 6th July 2011. The consultant and the author reviewed the wound and it was agreed to change the care pathway to larval therapy from 8th July 2011 until 27th July 2011.

Figure 1
On assessment, Mr C’s wound was 3cm x 3cm full thickness on the right knee the wound bed was 100% pink tissue and flush with the skin surface, with a cavity, where the original wound was. The cavity measured 1.5cm x 1.5cm and 1.5cm deep, but 100% pink and clean. The author took a photograph of the wound (see figure 1). The care pathway was changed on the 27th July 2011 to Sorbsan Ribbon ( Aspen Medical Europe Ltd) and Advazorb® (Advancis Medical) foam dressing, with Mr C visited every 48 hours.

Figure 2
Mr C was reviewed on the 17th August 2011 in Fracture Clinic. On assessment the original wound on the right knee had decreased to 1.5cm x 1.5cm. The wound bed was 100% pink tissue, flush with the skin surface, with a cavity still present, which was 1.5cm x 1.5cm and 3cm in depth. The wound was 100% pink and clean (see figure 2). The author took a photograph of the wound. The same dressing regime was continued of Sorbsan Ribbon and Advazorb® , with Mr C visited every 48 hours.
Case Study 2
Miss S, a 17 year old was referred to the author on 6th July 2011. The patient was originally admitted on 25th June 2011 with abdominal pain and subsequently went into theatre on 27th June 2011 for laparoscopy and pelvic abscess. Miss S was normally fit and well. On dressing removal there was a dehisced wound (15cm x 54cm) and 100% dusky pink. Her consultant was happy to proceed with the topical negative pressure dressing. She continued on this treatment regime until 25th July 2011.
On the 25th July 2011 Miss S’ wound was reviewed in clinic, and on dressing removal she now had a dehisced wound 13cm x 3cm full thickness, that started to heal well. On the abdominal wall there was some epithelisation at the bottom of the wound. The care pathway was changed from the topical negative therapy dressing to Sorban Ribbon, Aquacel (ConvaTec) and Biatain adhesive and C view edges to ensure a good seal.

Figure 3
Miss S was reviewed on the 27th July 2011. Her dehisced wound was 13cm x 3cm full thickness, but on the abdominal wall there was some epithelisation at the bottom of the wound. The wound bed was 100% pink granulation tissue. The wound exudate had completely filled the comparative foam with two dressings of 10cm x 10cm. The care pathway was changed to Sorban Ribbon, Aquacel and Advazorb and C view edges to ensure a good seal (see figure 3)

Figure 4
Miss S was reviewed on the 29th July 2011, the dressing was removed and the patient’s wound had decreased to 12.5cm x 2.5cm partial thickness. There was evidence on the abdominal wall of a large amount of epithelisation at the bottom of the wound bed, measuring only 0.5cm in depth and was nearly flush with the skin (see figure 4). The wound had still leaked a moderate amount of exudate but the Advazorb foam dressing had absorbed this exudate more effectively than the comparative foam.
Case Study 3
Mrs K was a 77 year old lady who underwent an amputation on her left leg on 26th February 2009. She was known to have Rheumatoid disease, arthritis and hypertension. Mrs K had a non healing ulcer for 3 years and the author had been managing her care for the last 2 years. The right outer gaiter area had a superficial ulcer 6.5cm x 5.5cm, the wound bed was 100% pink granulation tissue and 50% yellow tissue (see figure 5). The surrounding tissue was well perfused. A recent wound swab demonstrated Staphylococcus Aureus light growth and pseudomonas light growth that did not require any treatment with antibiotics. On 1st August 2011 Mrs K commenced on the Advazorb foam dressing for its soft and hydrophilic foam under reduced compression. She continued to have her lower leg washed and moisturised at each dressing change every 4 days.
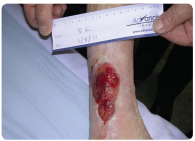
Figure 5
Mrs K was reviewed on the 5th September 2011. The right outer gaiter area had made substantial progress since her last clinic visit a month ago. There was now healthy granulating tissue and there had been a dramatic reduction in the size of the wound (3.5cm x 2cm), with 100% superficial pink granulating tissue and flush with the skin. (see figure 6).
Figure 6
The wound edges had epithelisation tissue present. The surrounding skin tissue was well perfused and moisturised. The small ulcer just above the ankle had completely healed. Mrs K was extremely delighted with just one month’s treatment. She found the dressing extremely comfortable and easy to remove.
Results
The results of these three patient’s case studies have been reported in full in this poster, with the patient’s outcomes. The patient’s experiences have demonstrated that they found the Advazorb foam dressing very comfortable and shows how the Advazorb foam dressing managed exudate. The patients did not experience any leakage of exudate using the dressing, so no loss of dignity was experienced. The case study on an abdominal wound demonstrated that the wound had produced a moderate amount of exudate, but the Advazorb foam dressing absorbed exudate more effectively than a comparable foam. The orthopaedic case study demonstrated that the wound had reduced in size within a month and the patient reported less exudate on the Advazorb foam dressing.
Discussion
The new Advazorb foam dressing appears to provide the optimum environment for healing. One lady had a chronic wound that had increased in size prior to the use of the Advazorb foam dressing, but substantially reduced in size within 4 weeks. It appears that the Advazorb foam dressing helps to prevent infection and the fluid from the wound is wicked away into the dressing. The patients commented on removal of the dressing as experiencing no pain. The nurses stated that in comparison to their usual comparable foam dressing, which they usually employed to manage these wounds, against Advazorb foam they found it very comparable. They concluded the Advazorb foam dressing provides an increase in performance to manage exudate, which appears to help promote wound healing.
Conclusion
Whilst this evaluation only contains three patient case studies, the patients found the dressings extremely comfortable and the author found them easy to apply and remove. There was improvement in all three case study wounds. The author was very impressed with the Advazorb foam dressing’s ability to take up the exudate compared with other similar foam dressings that were normally employed.

